Prevention and detection of cancer are two separate concepts.
Prevention (or primary prevention) means eliminating the conditions for any cancer to succeed (as in the example of cervical cancer that is preceded by many years of precancerous lesions, which are picked up by the smear tests and then treated). Detection (or secondary prevention) means diagnosing a cancer before the symptoms appear and so it is in a very early stage of development (though impossible to avoid). Preventive medicine is a major element in our medical activity (particularly for gynecologists).
For detection to be efficient the following are important:
- The cancer should be one that is sufficiently frequent.
- The cancer should be a public health focus in terms of morbidity and mortality.
- Detection tests should be best at isolating patients with that cancer.
- Detection tests should appropriate in terms of patient invasiveness and the financial cost to society.
For some years now, oncogenetic consultations are being held in France and throughout the world in order to help treat patients who appear to have a hereditary predisposition to developing cancer. These meetings hope to identify through the family case histories which cancers appear to have a genetic origin and then set about testing, using molecular biology techniques, for specific gene mutations (such as for example BRCA 1 and 2).
| Women with cancer (France) | 1980 | 1985 | 1990 | 1995 | 2000 | 2005 | |
|---|---|---|---|---|---|---|---|
| Breast | 21,704 | 25,140 | 29,649 | 35,392 | 42,000 | 49,814 | |
| Gut | 11,522 | 12,601 | 13,709 | 14,872 | 16,041 | 17,500 | |
| Cervix | 5,136 | 4,431 | 3,939 | 3,576 | 3,295 | 3,068 | |
| Uterus | 4,287 | 4,427 | 4,640 | 4,912 | 5,274 | 5,774 | |
| Ovary | 3,403 | 3,613 | 3,818 | 4,023 | 4,218 | 4,375 | |
| Lung | 1,595 | 2,031 | 2,647 | 3,537 | 4,825 | 6,714 |
Female cancers from 1980 - 2005 in France. (Note that breast cancer and lung cancer are the two cancers that are rising) Source INVS (Institut de veille sanitaire - French Health Care Institute).
Female cancer mortality rates
L’INCa (Institut National du Cancer, National Cancer Institute) has recently published jointly with the INVS and the CépiDC (Centre d'épidémiologie sur les causes médicales de décès, Epidemiology and causes of death centre) a report on cancer mortality in France:
“The development of major cancer mortality rates in France”
We highlight the female cancer figures for you to consider.
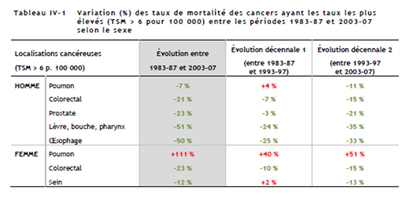
The first table shows the situation from 2003-2007. We included male prostate cancer numbers by way of comparison. We also retained lung cancer data since this is on the rise (we shall come back to this).
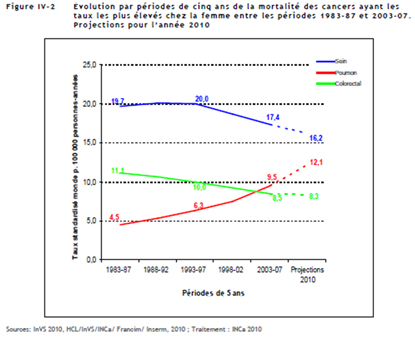
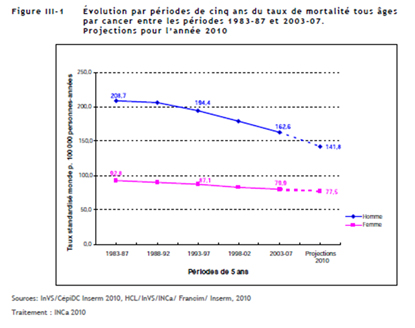
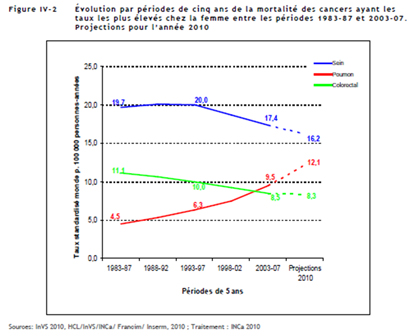
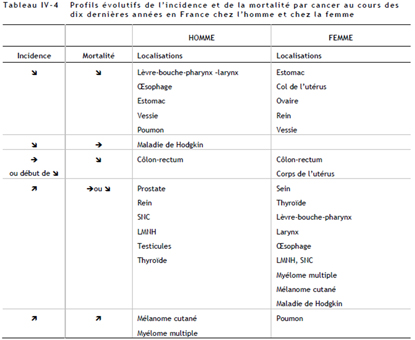
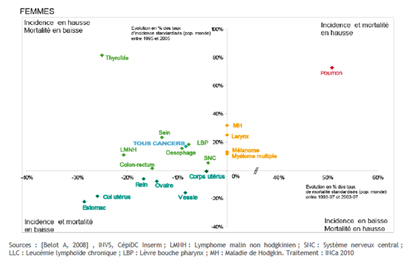
It is important to note that for most female cancers, both the incidence and the mortality rates are falling. However one cancer stands out in a negative way, lung cancer. Whilst lung cancer is falling for males, it is rising dramatically for women both in terms of incidence (+111%!) and mortality. By 2012-2015 we may even see lung cancer (rates are rising) overtaking breast cancer (rates are falling) as the number one female cancer.
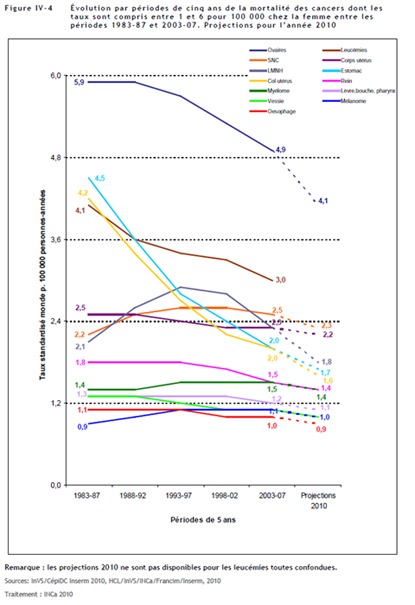
As regards specifically female cancers such as cervical cancer both incidence and mortality rates are significantly lower (down 52% between 1983-87 and 2003-07). This tendency appears to continue through 2010.
Lower rates continue for endometrial cancer which is down 8% and ovarian cancer which is down 4% in terms of incidence and down 17% in terms of mortality.
However, one other cancer is on the rise for both men (+45%) and women (+22%) and that is melanoma.
The tables below show in two dimensions female cancer tendencies.
For more please see:
http://www.e-cancer.fr/[...]principaux-cancers-en-france-novembre-2010
| Table I: Annual average number of deaths, standardized mortality ratio (SMR) and average age (Age) of death caused by the major cancers, period of study: 2003-2007 | |||||||
| Cancer locations | |||||||
| MALES | FEMALES | ||||||
| Number | SMR | Age | Number | SMR | Age | ||
| Lung | 21,650 | 42.9 | 68 | 5,870 | 9.5 | 69 | |
| Prostate | 9,120 | 13.2 | 80 | - | - | - | |
| Breast | - | - | - | 11,260 | 17.4 | 71 | |
| Cervix | - | - | - | 1,120 | 2.0 | 64 | |
| Uterus | - | - | - | 1,880 | 2.3 | 76 | |
| Ovary | - | - | - | 3,310 | 4.9 | 73 | |
| The average age of death is the age at which half of a population of women or men died. TSM/100.000 Sources : INVS, CépiDC Inserm, 2010 |
|||||||
| Table I I -2 Annual average number of deaths and standardized mortality ratio (SMR) caused by the major cancers, 2010 study | |||||
| Cancer locations | |||||
| MALES | FEMALES | ||||
| Lung | 21,000 | 38.6 | 7,700 | 12.1 | |
| Breast | - | - | 11,500 | 16.2 | |
| Cervix | - | - | 940 | 1.6 | |
| Uterus | - | - | 1,900 | 2.2 | |
| Ovary | - | - | 3,130 | 4.1 | |
| Prostate | 8,790 | 11.2 | - | - | |
| A specific method was used to estimate the number of deaths from cervical cancer and uterine cancer separately. (Belot et al. RESP 2008) Sources : HCL/InVS/INCa/Francim/Inserm, 2010 |
|||||